Case report of top executive team: What measurable change can a Sapiens program drive?
This article summarizes outcomes from a group of senior executives in Germany (n=32, each leading teams of a total of 200 to 5,000 people) who completed a Sapiens program together. Participants completed the Sapiens diagnostics as a baseline measurement, engaged in one-on-one and group interventions focused on personal health and energy management for 6 months, and then repeated the same diagnostics to quantify changes.
Sapiens is currently working with university partners on an academic publication evaluating impact in a large-scale client program over 18 months. Until that work is finalized, the results below describe an internal, unpublished pilot dataset.
Baseline measurement
During an offsite, participants completed the four components of the standard Sapiens diagnostics:
- Hair sample (3 cm hair, reflecting ~3 months) to measure hair stress hormones
- Two days of saliva cortisol profiles (3 samples per day: straight after waking, 30 minutes later, and just before bed)
- ECG monitoring across one representative workweek after the offsite (selected to avoid international travel and recent infections)
- A comprehensive self-assessment using scientifically validated questionnaires
In addition, participants could upload recent laboratory blood tests (if available), including markers such as lipids, long-term blood glucose (HbA1c), and inflammation markers (hs-CRP).
Results of the baseline measurement
About 1 to 2 weeks after testing was completed, each participant received:
- Their Sapiens report, including their Body Reserve Score ("the price their body pays for chronic stress")
- A 45-minute expert debrief to co-create a personal resilience plan
The report combines biomarker-based and symptom-based insights, including an in-depth view across seven body systems using scientifically validated symptom questionnaires (including gut, immune, musculoskeletal health, and mental health). Participants also received a structured view of current habits, work-environmental factors, and thought patterns. Individual results were compared with aggregate peer-level patterns, without disclosing anyone’s personal data.
Together with the expert, participants defined their personal action plan across intervention areas such as circadian rhythm alignment (timing of daily activities), nutrition, movement and exercise, and self-regulation techniques (for example breathing, body tension release, and mental strategies related to stress and resilience).
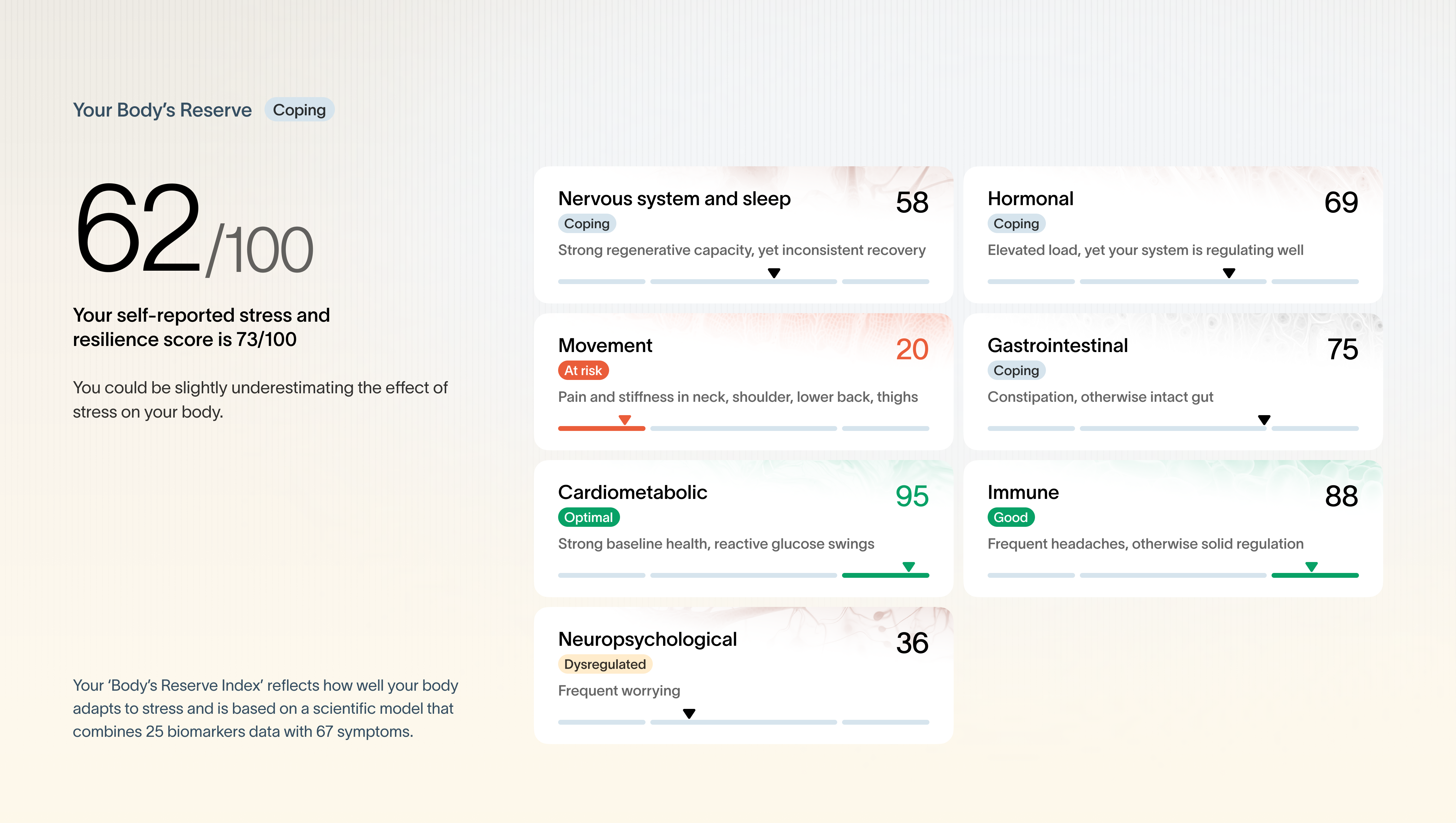
While each individual showed their own strengths and challenges, several patterns appeared across the group:
- Elevated evening cortisol for the large majority of participants
- Elevated evening activation levels in the ECG-based HRV analysis
- Low sleep quality, reflected in an average recovery during sleep of 58% per night (with >80% considered optimal)
- For around half of participants, a blunted morning cortisol awakening response, which may indicate insufficient night-time recovery and/or a misaligned circadian rhythm
In expert conversations, many participants described back-to-back meetings during the day followed by desk work late in the evening, which may have contributed to a late activation pattern. This was often described alongside late and heavy dinners and family conflicts related to work vs. family time, which may have intensified evening activation and wind-down challenges.
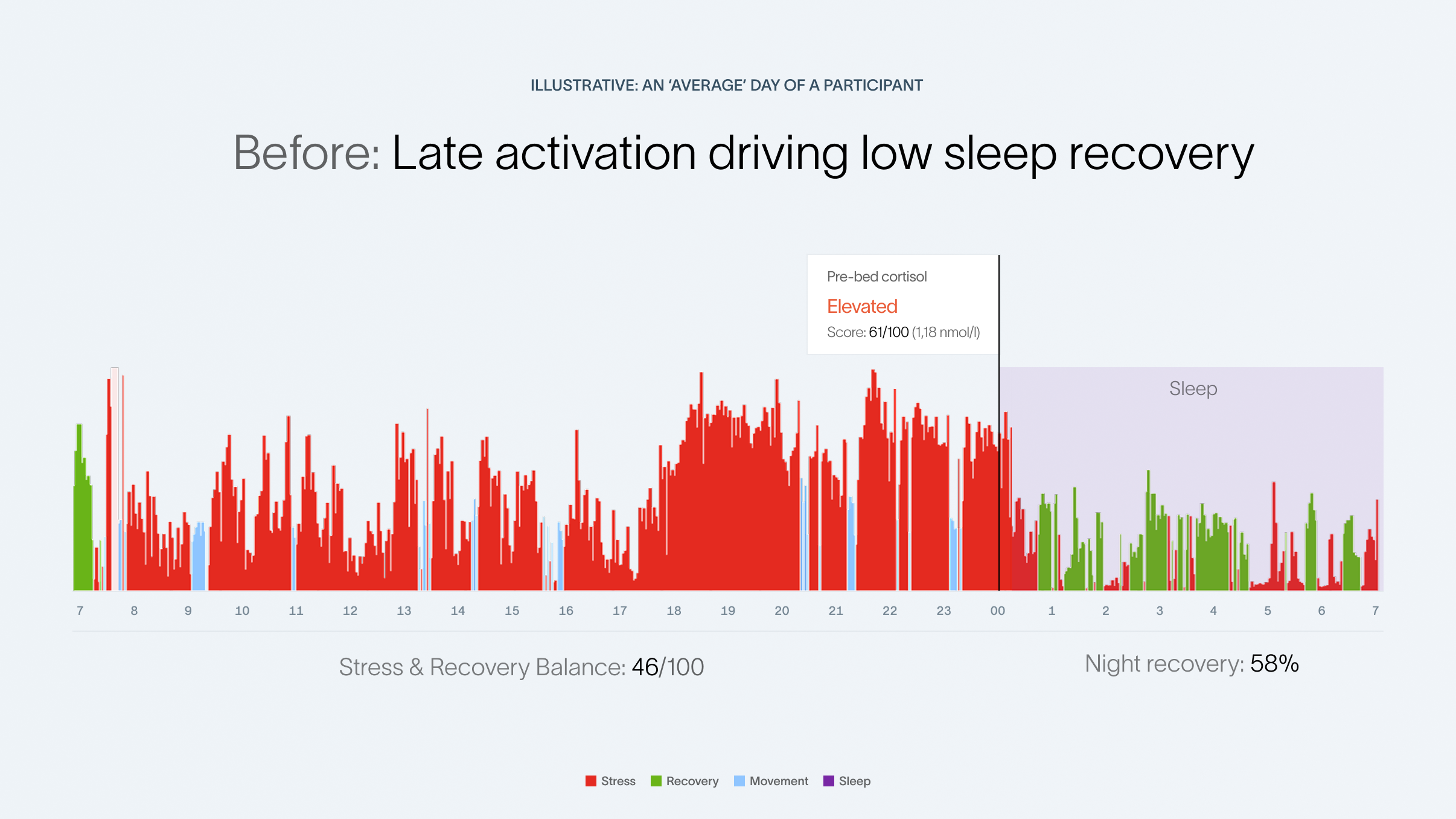
Interventions
Across 32 participants, commonly selected interventions included small behaviour changes in their work- and lifestyle.
Recovery and sleep
- Morning outdoor light (aiming to address a blunted morning cortisol awakening response)
- Switching off devices 30 minutes before sleep
- Meditation before sleep
- Rhodiola rosea (aiming to reduce cortisol)
Nutrition
- Protein- and fiber-rich breakfast
- No coffee after lunch (aiming to support sleep quality)
- More mono-unsaturated fats and omega-3
- Protein-rich afternoon snack (aiming to reduce late dinner meal size)
Many participants also reported metabolic health challenges (for example elevated long-term glucose/HbA1c values in uploaded blood tests), which informed nutrition priorities.
Other commonly selected interventions (based on personal data and goals)
- Movement: post-lunch walk; morning micro-workout; 10+ minutes of high-intensity exercise per week
- Attention regulation: working in 90-minute blocks; first 30 minutes of the day without phone; 1-minute body scan practice before meetings
- Emotional regulation: 1-minute down-regulation before meetings; mental reflection with 3 questions; scheduled worry time after work
In addition to individual debriefs, participants joined workshops to practice self-regulation and build skills across core resilience domains:
- Biofeedback training (breath, body tension, vision)
- Nutrition masterclass (personalization to individual situation and challenges)
- Evening wind-down, sleep, and jet lag management masterclass
- Attentional regulation and mental fatigue masterclass
The Sapiens team supported the participants with regular personal check-ins, group calls and peer-group support to increase the chances of implementing these committments during the period of 6 months.
Results after 6 months
Six months later, participants repeated the same measurements. The group trend of elevated evening cortisol and elevated evening nervous system activation had been partially addressed.
Key results after the 6 months interventions:
- Reduced evening cortisol for most participants
- Mean saliva cortisol before bed decreased from 1.18 nmol/L at baseline to 0.76 nmol/L at 6 months.
- This corresponded to a 26% improvement in the evening cortisol score (an index comparing absolute cortisol values to reference groups adjusted for biological sex and age).
- In simplified program language, this was translated as a 26% improvement in wind-down.
- Improved recovery during sleep
- Average recovery during sleep improved by 16%, from 58% per night to 67% per night.
- Improved stress–recovery balance (HRV, ECG over 5 workdays)
- Stress–recovery balance improved by 28%, from a score of 46 to 69.
- Improved hair markers (retrospective ~3-month view)
- Hair-based markers improved from an average score of 48 to 62 (a 29% improvement).
- This reflected a normalization pattern: some participants with cortisol significantly below norms for their age group increased/normalized, while others with excessive cortisol reduced.
Sapiens, through a self-assessment, controlled for work demand which was assessed by participants for themselves on a scale from 0-10 as well as by asking for the average working hours in the past 8 weeks.
The work demand, based on these 2 metrics, stayed the same during the measured period.
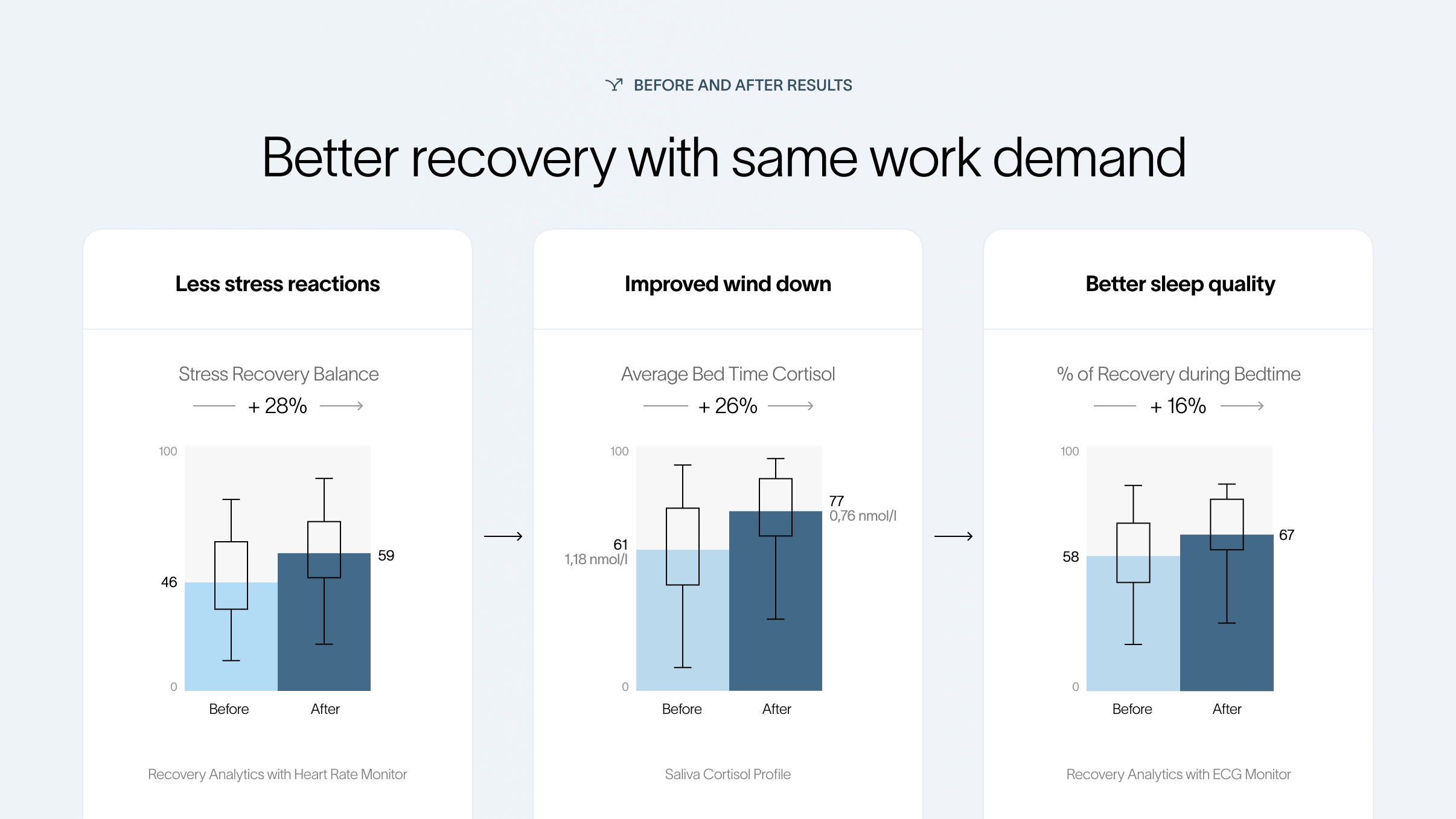
The personal shift: 'Health' as an attitude
More important that the aggregate shifts in the biomarkers was the shift towards 'health as an attitude'. People report that they feel more energy, less fatigue and are more ready to address their leadership challenges.
Based on similar case reports and a scientific literature analysis, we calcualted that a productivity increase of 7% can be expected from such a shift in health (yet, for executives productivity remains difficult to define and measure).
For many participants, an average day looked more like this after the 6 months Sapiens program:
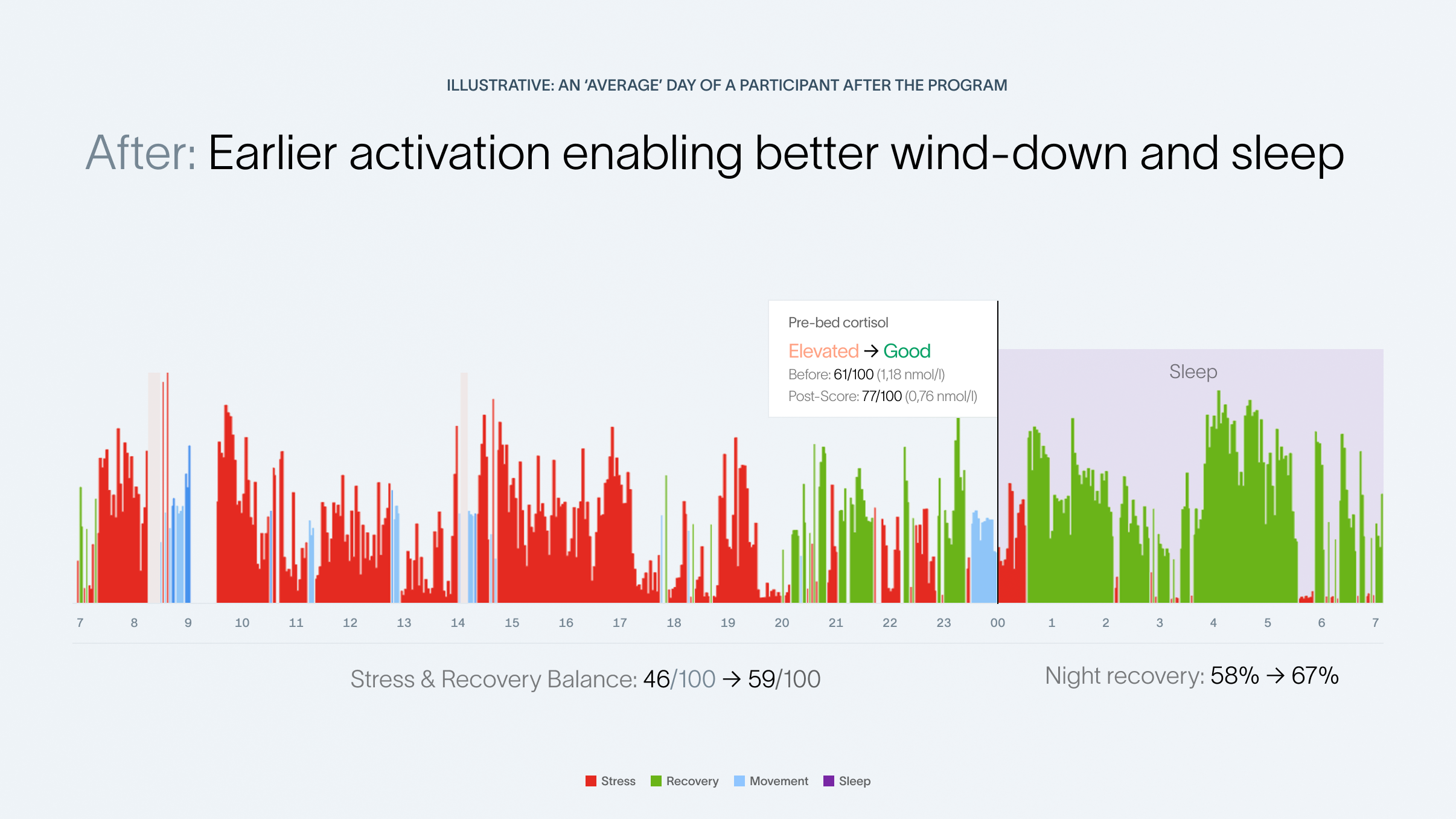
Limitations and interpretation
Sapiens is currently working with university partners on an academic publication evaluating impact in a large-scale client program over 18 months. Until that work is finalized, the results below describe an internal, unpublished pilot dataset.
- Sample size: The sample is still insufficient to claim statistical significance. At the same time, the longitudinal follow-up and the breadth of data from 32 participants shows a measurable trend across multiple diagnostic layers.
- Team context: Because participants worked together day-to-day, a key strength of the company format may have been peer support in reaching health goals. This dynamic may contribute to observed changes beyond the official interventions.
- Seasonality: Seasonal effects were not adjusted for. Data were aggregated from two cohorts: one cohort measured from November to May, and the other from May to September.






